By Ray Deshaies
Beginning with the introduction of aspirin at the start of the 20th century, there have been three major waves of innovation in drug discovery. We are now at the start of a fourth wave that will radically alter our concept of how drugs can work, paving the way for new treatments aimed at thousands of disease targets now viewed as undruggable."
Show Transcript
To appreciate the staggering potential of this emerging paradigm shift, let me briefly describe the first three waves and their impact on modern medicine. Wave 1, launched by aspirin, gave us medicines with well-defined chemical structures but unknown biology. They worked, but we didn’t know why they worked. In the 1970s, Wave 2 introduced rational drug design—specific compounds aimed at specific molecular targets that play a role in disease. Drug hunters finally knew not only what they were making but how it achieved its effects. The 1980s ushered in Wave 3, the biotechnology revolution. Recombinant DNA technology allowed us to go beyond chemical compounds and design medicines based on the proteins and other large molecules that govern biology.
While transformative in many ways, these innovations didn’t really change our basic idea of how drugs should work. In nearly every medicine approved dating back to aspirin, you have one molecule—your drug—and another molecule—your target. The drug binds to the target in a manner that changes the target’s normal activity. The drug itself does all the hard work of dialing the activity up or down, most often down. That’s drug design in a nutshell. Conceptually, it isn’t very complicated.
Future medicines could function very differently. In biopharma pipelines across the industry, we’re seeing more investigational multispecific drugs that can form connections with two or more proteins. They include some highly sophisticated structures that function as molecular matchmakers. Instead of engaging targets on their own, these agents mobilize biological mechanisms to do the heavy lifting. By inducing proximity between their targets and these mechanisms, multispecifics can harness the awesome power of biology to go well beyond what conventional drugs can accomplish. This isn’t an incremental improvement in drug design, it’s a sea change.
The molecular version of a recycling sticker
Nature’s playbook offers good examples of what induced proximity looks like in action, including some clever viruses that can commandeer the cell’s protein disposal system. When a cell wants to get rid of a protein, it uses specialized enzymes to tag the protein with ubiquitin—a molecular version of a recycling sticker. When ubiquitin-tagged proteins encounter a cellular machine called a proteasome, they get pulled inside and chopped into little pieces. Some viruses have learned how to thwart the cell’s antiviral proteins by making molecules that link these proteins to ubiquitin-tagging enzymes. Basically, they trick the cell into trashing its own defenses.
Drugs that can accomplish this same trick are called PROTAC® molecules (proteolysis targeting chimeras). A few medicines, including the successful cancer drug lenalidomide, were discovered to function in this manner only after they were approved and on the market. Now there are several companies investing in research into similar molecules, attracted by the large advantages these potential therapies might provide.
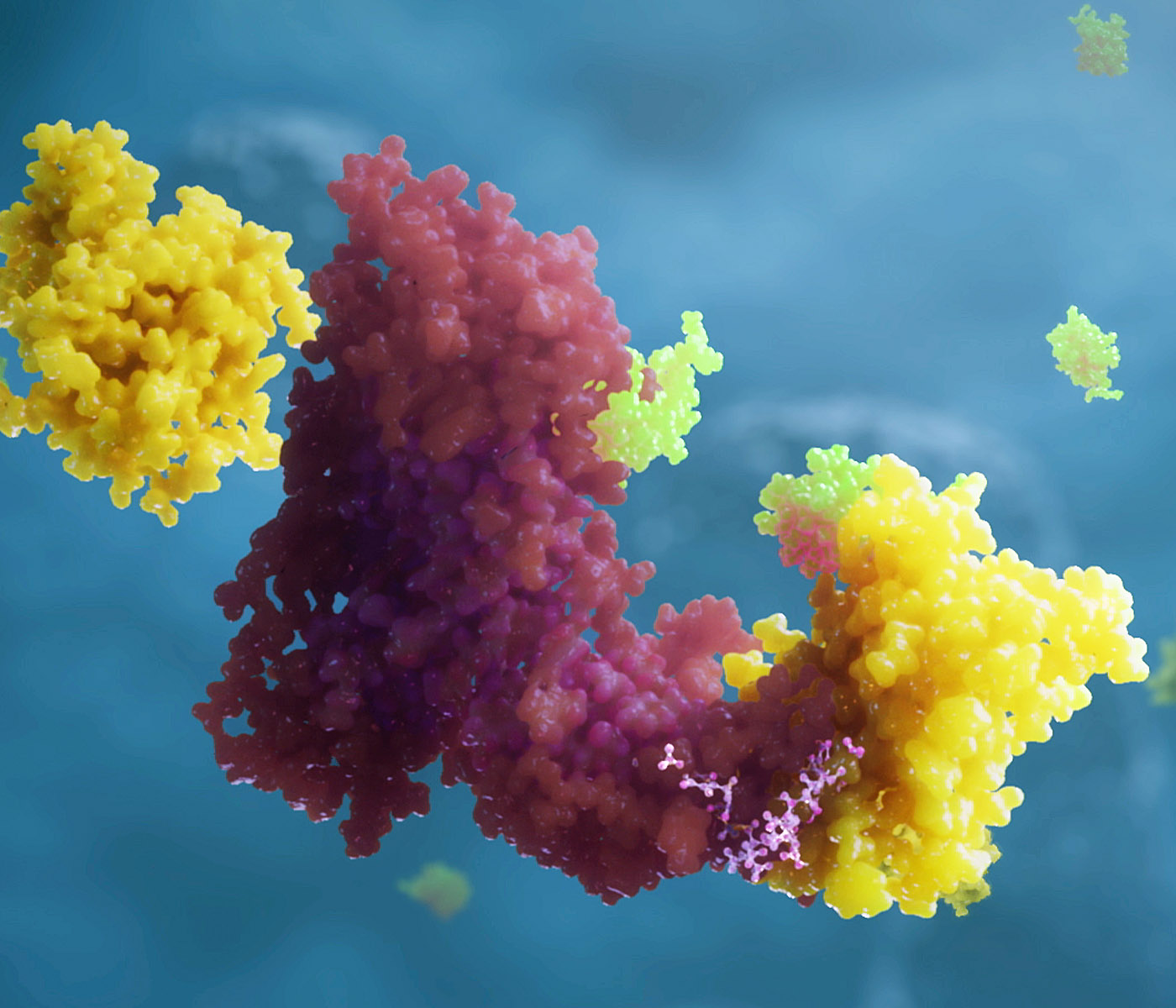
A PROTAC (small pink molecule, lower center) works by bringing a target protein (shown in yellow) into proximity with enzymes known as ubiquitin ligases (purple). Once in proximity, the enzyme attaches a small protein called ubiquitin (green) to the target protein, which marks the target for degradation.
For starters, a conventional drug only works for as long as it’s binding to its target. The instant it loses its grip, the target goes back to causing disease. A PROTAC molecule doesn’t need to remain in contact with its target because one encounter can trigger the target’s irreversible destruction. What’s more, just one of these molecules can take out multiple targets sequentially. Its effects are more durable because the target is gone until the cell can make more of it, which takes time. More importantly, these and other types of induced proximity agents could overcome a big limitation that narrows the range of targets current drugs can hit.
Just as a key needs a matching lock to work, conventional drugs need targets with binding pockets that are essential to the target’s activity. Proteins lacking functional pockets that drugs can nestle into are deemed “undruggable”—and about 85 percent of human proteins fall into this category. However, since the effectiveness of PROTAC molecules come from the enzymes they bring to the party, their usefulness isn’t restricted to the 15 percent of proteins with functional pockets. Instead of fitting like a key in a lock, they can use any binding site that allows their companion enzymes to do their job.
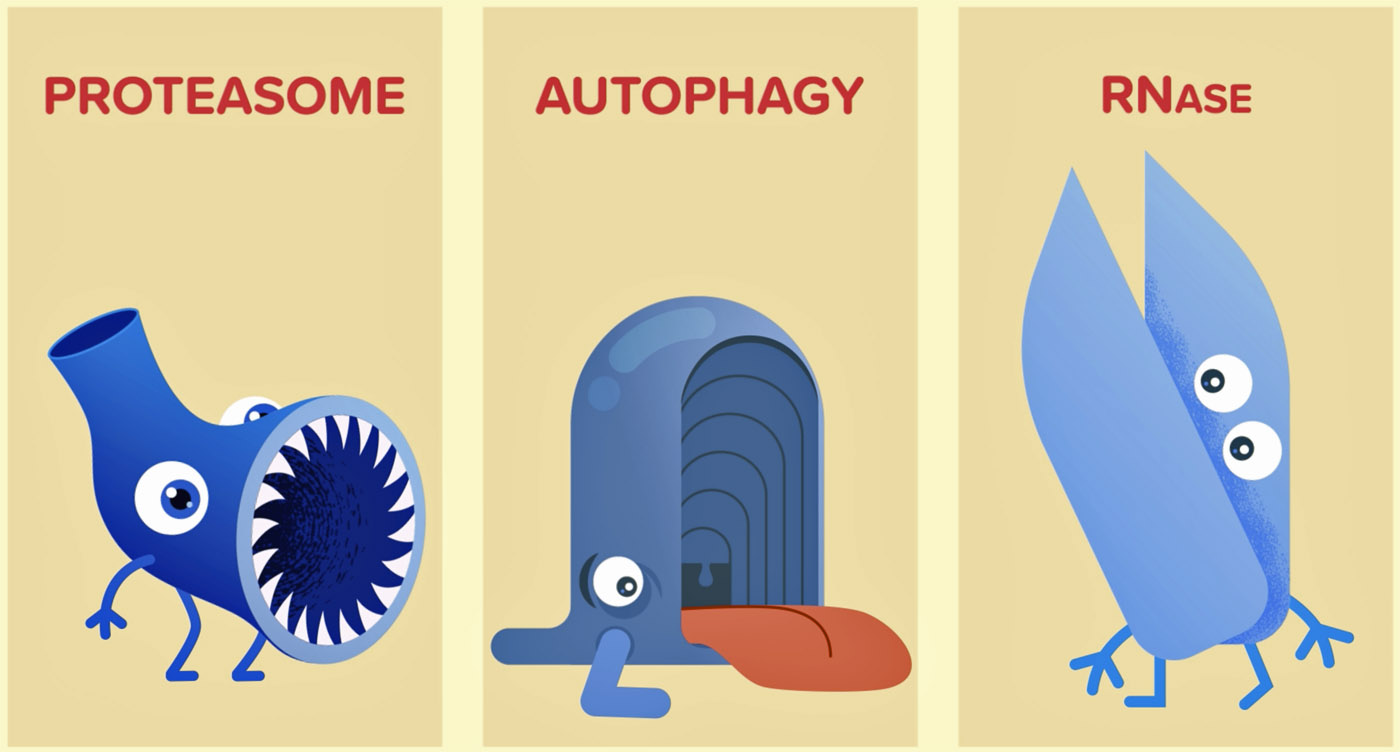
Induced-proximity agents could be designed to enlist the machinery our bodies use to degrade proteins, gobble up cellular debris, and slice and dice RNA that cause disease.
Limitless possibilities
PROTAC molecules are just the tip of the iceberg in terms of the matchmaker molecules we could design. In biology, countless mechanisms work through induced proximity, which means there are countless ways for drug hunters to try to treat disease by exploiting this approach.
- Already, we’re seeing early descriptions of “LYTAC” molecules, which can link targets in the blood to the receptors that cells use to capture and recycle unwanted proteins.
- The target doesn’t need to be a protein. Cells have specialized machinery to eliminate unwanted RNA, the nucleic acid that translates DNA into proteins. “RIBOTAC” molecules could eliminate specific RNA sequences linked to disease proteins.
- We could also design “AUTAC” molecules that leverage a process called autophagy (literally, “self-eating”) that cells use to gobble up unwanted debris, like clumps of sticky proteins and damaged organelles.
The potential for generating new combinations and new biology is endless. We’re only limited by our technical capabilities, vision, and creativity.
At Amgen, we addressed a key technical need in 2019 by acquiring Nuevolution, now Amgen Research Copenhagen. The scientists there are world leaders in building DNA-encoded libraries. This technology uses DNA tags to barcode individual chemical compounds in huge mixtures of billions of different compounds. The Copenhagen team has built libraries that collectively hold 40 trillion unique compounds. That massive collection will help us to find those one-in-a-billion compounds needed to reach the high-hanging fruit of potential drug targets using multispecific molecules.
This isn’t the first time Amgen has sought to build a highly promising platform technology. In 2012, we acquired Micromet, which pioneered a new type of therapy known as bispecific T cell engagers, or BiTE® molecules. These molecules work by inducing proximity at the cellular level, bringing T cells together with tumor cells so the former can recognize and destroy the latter. Eight years after that acquisition, we have one approved BiTE therapy, additional BiTE molecules targeting seven types of cancer now in clinical trials, and third-, fourth-, and fifth-generation BiTE structures at the design stage. In the decade ahead, we hope to make similar progress with our small molecule induced proximity platform.
The urgency of this effort is underscored by many discoveries emerging from human genetics and allied data. These technologies are revealing that numerous genes and proteins that lead to disease are linked to targets that can’t be drugged by any conventional medicine. Multispecific molecules have the potential to expand the universe of druggable proteins from just 15 percent to nearly 100 percent. This new wave of innovation makes it possible to imagine a day when many more diseases can be treated or even cured.
Click here to view the full Amgen Induced Proximity Platform Fact Sheet.







